 Discover the latest biohacks to decreasing neck and back pain! In today’s episode, we are going to discuss the most common causes of back and neck pain that you may not even be aware of. Dr. Jason Hamed and Dr. Bryan Joseph introduce the concept of non-surgical spinal decompression and how that has helped thousands of patients get well and stay well.
Discover the latest biohacks to decreasing neck and back pain! In today’s episode, we are going to discuss the most common causes of back and neck pain that you may not even be aware of. Dr. Jason Hamed and Dr. Bryan Joseph introduce the concept of non-surgical spinal decompression and how that has helped thousands of patients get well and stay well.
Table Of Contents
- Introduction To Non-Surgical Spinal Decompression
- Dr. Jason on TV: Back Pain & Spinal Decompression Overview
- Why We Experience Back Problems
- Changes In The Spine For Someone Who Has Back Problems
- Biohacks For Inflammation & Spinal Decay
- Supportive Care After Non-Surgical Spinal Decompression
- Closing Thoughts: Take Care Of Your Back
Introduction To Non-Surgical Spinal Decompression
Bryan Joseph: Beautiful day here. Actually not so beautiful.
Jason Hamed: Actually it’s not really beautiful. But as your wife’s father says, as long as it’s sunshiny inside your head. So, that’s what he says. I love that. I’ve thought about that. It’s crappy outside, actually. It’s like we have to get a nap.
We got a little overcast, rainy day, but no, that’s not going to impact the message we’re going to share with you today. This is episode 38 and, as always, we thank you for continuing to listen to the show and spread the seeds and the messages to other people. We started this with the pure purpose of just trying to help more people get well and stay well and you know, ironically that mission because of you, is continuing to unfold and we thank you for that.
So today we’re going to talk about something that we’ve got a lot of experience. You know, really it’s in our wheelhouse because this is what our backgrounds are in, especially when we went through chiropractic school. Most people are most familiar with chiropractic, actually solving people’s neck and back issues. So what we wanted to dive a little deeper on today was just have a discussion around some of the latest, you know, we call them bio hacks for back pain, which basically are shortcuts or things to be aware of.
Dr. Jason on TV: Back Pain & Spinal Decompression Overview
Talking About Spinal Decompression and Back Pain
Dr. Jason was recently featured on our local TV “Great Day St. Louis” show, and the above video is a great explanation and overview of what we will be covering in this episode.
Why We Experience Back Problems
Bryan Joseph: So, why don’t we break this out by first starting off with the most common reasons or causes as to why, in your opinion, after now practicing for 16 years as a chiropractor, why do you believe most people experience back issues?
Jason Hamed: Sedentary lifestyle.
I mean, not like that’s it, but I can expand on that exponentially in different directions. We just sit too darn much and it literally is creating, and we’ve talked about this in multiple podcasts … You know, we even talked about how your body molds into this position of the chair. Like, you literally become the chair, like literally. And then you’ve got overly tight muscles in the front of your body, like specifically your pec muscles, that’s your chest. You’ve got weakened muscles in the back of your shoulders and neck. You’ve got chronically tight muscles in the front of your hips. They call them the hip flexors, and you’ve got no strength in your butt muscles whatsoever. You’ve got chronically tight, low back muscles and a weak core. And that comes from sitting. We don’t get that when we’re kids.
You got the young kids, I got young kids, you watch them go out and play and they’re moving vigorously. Most of their day, they’re moving. And then we get transitioned into adulthood and we just slowly, it’s like a slow death, we stop moving. And we actually like, movement becomes such a rarity as we become adults, versus when we’re kids we move more than we stop.
We stop more than we move
Jason Hamed: Then when we’re adults we stop more than we move. And then when we do move, like golf, and then follow up our day at the gym, our body gets freaked out. Like that’s it. Like, I mean we could split hairs and we could go and talk really, really scientific and whatnot, but at the end of the day is, we stop more than we move.
Bryan Joseph: So I would actually put that in a category that we talk about a lot, which is basically sitting is actually acting as a stressor to your body, right? I believe in many, many, many capacities and I think you agree with me, that almost all forms of destruction to the body really can be broken down into stress and it can be physical stress as we’ve talked about, emotional stress, even biochemical stress or other different types of infections that can be, you know, a stressor. But let’s talk about physical stress a little bit because when you’re talking about sitting or sedentary lifestyle, we don’t think of that as a stress the same way that we might think of like a car accident, right?
Jason Hamed: Right.
Bryan Joseph: Or, I don’t score well on golf. So you know, taking well over a hundred swings, you know, after I hadn’t really warmed up the body or stretched out and just getting out there and whacking away, is a stress to the body. But equally, you know, not using your body and sitting all day long is considered a stress, if not a bigger stress than some of the other ones that I just mentioned.
Micro traumas around the spine due to stressors
Bryan Joseph: So what I hear happening in these, you know, yeah, we can go clinical and have deep discussions on these things, but ultimately these stressors or sedations of sitting all day long, they create micro traumas around the non-surgical spinal decompression, the spinal column itself. And the spinal column is made up of bone structures, it’s made up of tendons, it’s made up of ligaments, it’s made up of nerves, muscles, et cetera. And the more, whether it be major macro traumas or the or these micro trauma that you accumulate, the more likely that you’re going to create damage to these areas.
Jason Hamed: Your joints will literally fuse into that position that that cast was in. This is exactly the same physiology, the same type of science that’s going into when you sit at a desk all day long, slouched over. It may not be a cast, but you’re sitting there for hours doing that and you’re slowly lose … Your body is slowly losing its ability to move and it’s getting scar tissue around the joints just like in that cast. And if you don’t have a good therapist that’s going to help to get that joint movement back, you’re going to lose it, right? Now we’re just talking about the all the joints of the non-surgical spinal decompression doing the exact same thing.
Bryan Joseph: Now, you make me think of two things. Because again, this is all related to back pain and back neck, mid-back, low back, it doesn’t matter. It’s all one big system, one big ecosystem.
Hidden inflammations due to micro traumas
Bryan Joseph: You see that your body naturally knows what to do. It lays down scar tissue. Underneath the skin, the same thing happens. So when we start to get these micro traumas underneath the skin, whether it be a sprain or strain or just a little tweak here and there, what you can’t see is your body’s producing a lot of inflammation and it’s laying down these different scar tissue properties and it’s basically, you know, adhesing or thickening the tissue underneath the skin, which basically, what does that mean to you? That means you can’t move. You’re not as mobile or flexible as you once were, right?
Jason Hamed: Yeah. And the challenging thing is, is like the whole boiling the frog in the water. You know that little thing where you could put a frog in there and you slowly boil it. I don’t know if it’s a wife’s tale or not or if it actually is true. This is what’s happening, right? Because people don’t know that it’s these little micro traumas, these little scar tissue formations that are occurring.
You don’t feel it. But what happens is, you’re in these patterns of stressors of overdoing it or under-doing it and then you fast forward five, 10 years and you’re like, oh my gosh, I can’t even stand upright. I got this huge hump in my back. What’s this hump coming from? Or why is it that every time I cough, sneeze or use the bathroom, my back hurts. Or again, how come two years ago I could go play golf with my friends and my family and I didn’t hurt and then all of a sudden today I do, right? That’s it, man. It’s a slow death. It really is.
Changes In The Spine For Someone Who Has Back Problems
Bryan Joseph: Can you just take a minute to explain like, you know, two things that you typically see when we evaluate somebody that comes in that’s either had a history of back pain or currently experiencing it. When you take an x-ray, after doing an evaluation, clearly, as you mentioned, there’s probably going to be restricted motion, but can you describe some of the changes of the physiology you see on an x-ray that typically would match up.
Jason Hamed: So just think about a skeleton. Now think about all the Halloween times you’ve seen a skeleton or you’ve seen a little picture of a skeleton. The skeleton is supposed to be straight.
That’s a fact. Okay, so when you look at the backbone, okay? We call that the spine. When you look at that, it’s supposed to be straight, period. Now when we have slips, injuries, falls, accidents, sitting for hours and hours on end, times decades and decades and decades of emotional, physical, chemical stress that’s tightened up our muscles, tendons, and ligaments … What the byproduct of that is, Dr. Bry, is when you now look at an x-ray, it no longer is straight. It literally has a bend in it, okay? There’s technical terms for it, but just keep it real simple.
It’s got a kink in the spine and now, unfortunately, what that’s doing, that kink does two damaging things to people’s bodies. The first, we have delicate nerves, that come out of the little holes in between every one in the bones. Well, guess what? If you kink that non-surgical spinal decompression, what do you think you’re doing to that nerve?
Bryan Joseph: You’re going to put pressure on it.
Nerve damage & poor spine alignment
Jason Hamed: Right. You’re going to pinch that nerve, and if that nerve is pinched, it causes pain or it decreases the brain’s ability to communicate to the muscles around it. That’s why a healthy guy, a fit guy like you, can swing a golf club and the next day try to do a clean and jerk and he gets a tweak, because his brain wasn’t signaling those muscles the right way.
Bryan Joseph: So, let’s just make it real clear. I know who the jerk was.
Jason Hamed: Right. The other problem with that is the human body is meant to be in alignment to optimize movement. I tell patients, optimal alignment means optimal movement, good alignment, good movement, good movement, you’ll feel good, that’s it. So when your body has got these bends or these kinks in it, specifically at the non-surgical spinal decompression, it cannot move correctly. And when it can’t move correctly, it hurts.
Why does it hurt? You said it earlier, it creates inflammation, the joints start to wear down, and now we have a breakdown process called degenerative joint disease or degenerative disc disease. So again, alignment means good movement. Good movement means you feel good. If you don’t have good alignment, then guess what? You could go ahead and get every pill, potion, lotion on the planet. I love massage therapists, but you can get massages all day long, but if you don’t change the alignment and really correct it, you’re only going to keep coming back to a problem.
Spinal decay and how prominent it is
Bryan Joseph: So the spinal bones, when you’re talking about degeneration, are really, really similar to that, which means if your alignment of your spinal structure is favoring one side or the other for whatever reason, and that reason usually is one of those stressors we talked about in the beginning, then it’s going to put pressure on certain sections of the spine and force those to basically age at an accelerated rate, compared to some of the other spots. And that accelerated aging is really what you just mentioned before. That’s what’s called arthritis. That’s what’s called disc degeneration. That’s what’s called spinal decay. It’s got a lot of different names, but it basically means that there’s a section of your body breaking down faster than it’s repairing itself.
Jason Hamed: And how many times have you seen this? We’ve all seen this where someone walks in, they’re look super healthy, super fit. They’re like, doc, I hurt myself. Like you said, a weekend warrior, I hurt myself. We put up the x-ray, we sit down and discuss what we found with the patient and like their bones in the lower back look like someone 20 to 30 years older than the person who’s sitting right in front of me, right?
And then you have to have that conversation with them, which I totally understand. And I know you do, too, that they thought it just happened this weekend. But you have to have that conversation as a clinician and say, listen, actually this problem, based on this x-ray, alone, has actually been developing for about 20 some odd years or longer or even, you know, 10 years or something of that nature, because it’s chronic.
Is spinal decay connected with age?
Bryan Joseph: I used to think this way in many ways, well it’s just common. It’s old age, right? But the irony is when you look closer and you actually do a comprehensive evaluation and you study the x-rays, you look at all the individual bones and you say, man, you know reality is, three of them are really bad. Ten of them are really, really good. And are they all different ages?
Jason Hamed: No, because if it was just age, they’d all look like crap.
Bryan Joseph: Exactly, so naturally there’s some slow, you know, wear and tear that’s going to happen through the aging process, but what we’re talking about is basically some of the areas of the body that that turn into weak spots or weaknesses that actually show up in terms of back pain later.
Jason Hamed: I had a patient when we were first in practice. It wasn’t even my patient, it was my uncle because I was working in his office at the time. But I’ll never forget, he brought me in to look at her x-rays. It was a nun from a local a church in the area, out in Tulsa, and she came in and she had perfect alignment, literally, probably one of the best I’ve ever seen.
She had the normal curves from the side and she had like next to none as far as degeneration and she was in her 80s at the time. And yet, I had seen like maybe a 20 or 30-year-old come in that I was taking care of, that had a worse body than this 80-year-old nun. So it had nothing to do with age, but how that person took care of their frame over the years.
Biohacks For Inflammation & Spinal Decay
Bryan Joseph: Why don’t you just take a few minutes to just describe, you know, some of the things that you now are putting in place in regards to active protocols for different conditions and tools that you’re now becoming aware of that you think are cutting edge and beneficial for patients.
Jason Hamed: Let’s start with inflammation. The very first thing to put out the fire is there’s really nothing sexy. Use ice as much as you possibly can. I’m a proponent of like ice baths and freezing cold showers. So that’s something that each and every day that someone can be doing just to help decrease some of the inflammation that their body is going through.
Now you can use heating pads and heat as well, but you’ve gotta make sure that you’re marrying the two. So you’ve got to have a combo of heat and ice. If you only have time for one, I’m a huge advocate of just going ice. There’s a lot of people out there that talk about the role of heat and I get that, but I am just a sucker. I love the cold therapy. I just see a ton of benefits from decreasing inflammation, but it also helps to stimulate some growth hormone production, helps your body to mitigate different stress responses and improves breathing patterns.
Just fill a tub up with some ice, get in there, you know, get in and get out just so you can tolerate it if you can, or if you’re really struggling to get an ice pack on the lower back, get out of gravity as soon as possible. Those are my huge bio hacks to decrease full body or specific inflammation.
Get your body in the right alignment
Bryan Joseph: Now I want to be evaluated and I do find that I actually have a some misalignments or I got some poor structure-
Jason Hamed: Issues. So the first thing on this, is openly … And I know we can talk about bio hacks all day and I know I’m biased in this, but the best bio hack is getting your body in better alignment. Like, I could sit here and-
Bryan Joseph: How does one do that?
Jason Hamed: Well, first you got to know if it is in alignment, right? It’s like how do you get your cholesterol down? We’ve got to know if your cholesterol is even up, right? So you’ve got to get in and get an evaluation. In this office and what we do, what we specialize in and what I advocate for my friends and family is, get to a place that’s going to take a full spine x-ray so they can look at you from top to bottom. Because even though you have lower back discomfort, believe it or not, some of the challenge, if not many of the challenges, may be originating from your mid back into your neck because it’s laws of physics. Like you said earlier, it’s one big ecosystem.
Bryan Joseph: It’s like the leaning tower of Pisa.
Jason Hamed: Exactly right, man, right.
Bryan Joseph: The bottom is a little off, but then the top is way off.
Jason Hamed: A hundred percent, brother. So first you’ve got to know what your alignment is or what it isn’t and then once you do that, and we actually have a way to measure where the alignment is and isn’t it, then you got to go through a process of correcting it.
Corrective chiropractic adjustments
Jason Hamed: Now again, what we do, and I can only speak of what we do and others do similar type of work, is we do what we call corrective chiropractic work, where I’m looking at where your misalignments are or someone’s misalignments are, and then we’re looking to put something called an adjustment.
A gentle, but very specific force into the body to slowly get it to nudge closer to optimal or normal. And then we support that with different therapies in strengthening work to make sure the muscles, tendons, and ligaments can actually hold that alignment. And then there’s going to be some frequency, openly, because you can’t change a habit just with one day, one treatment.
So when you have the repetition over time, you can actually recreate a new habit and retrain the body. The same way that someone retrains their body to be looking like their chair, we can now actually train it to look more like optimal or as near as normal as possible.
Bryan Joseph: Well, I think more commonly, the same way that somebody would go to a gym and train their body to try to get in better shape physically, it’s that repetitive training that you’re doing that eventually starts to get momentum and builds the physique that you’re looking for. So chiropractic care, ice bath, some rehabilitation associated with the chiropractic care if there’s alignment issues, what if there’s damage to the disc?
Non-surgical spinal decompression
Jason Hamed: That’s where we have to use a more advanced protocol. That’s when we’re looking at non-surgical spinal decompression. So, our patients that will come in with that, and even friends in different parts of the country, I’ve advised this, you’ve got to find out what your alignment is and fix it. But the same token is, you also have damage to the disc now. You’ve got to address that at the same time.
Bryan Joseph: To be clear, the disc is the space between two bones in your back. And just like the tire on the car starting to wear out, one of the most common spots that we see wear out, when we take x-rays of the spine, is that disc, that cushion between two bones.
Jason Hamed: Like Dr. Bryan said, it’s an ecosystem. It’s not one disc does all the load for your neck or takes all the pressure off your lower back, but it’s all of them work together as a team. When you have these challenges, when you have some of these breakdowns this degeneration you alluded to, that cake of the donut becomes weak and brittle and now all of a sudden that jelly can squirt out and this is what we hear when people have a herniated or a bulging disc.
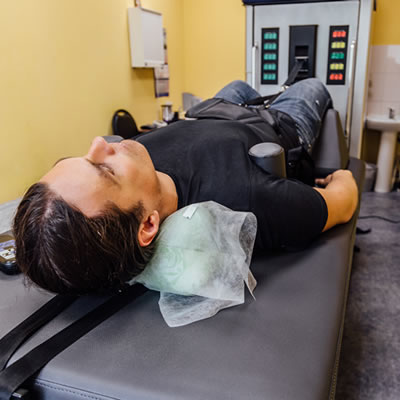
And so the only way we can actually fix that naturally is to use something called non-surgical spinal decompression. And that’s the device that you can lay on. We have a big table here in the office and you get strapped into some harnesses that we can specifically target which level of the disc is herniated, just by gently and very relaxing, just open the spine up and it allows the disc to self-absorb and come back in.
Supportive Care After Non-Surgical Spinal Decompression
Bryan Joseph: So we’ve gotten inflammation and pain under control. We’ve been working on correcting our alignment through doing some rehab and chiropractic adjustments. We have some degeneration or some damage to our disc, so we’re going through non-surgical spinal decompression. Now we’ve got all that in relatively a healthy state and we don’t want it to repeat itself, so what do we do in terms of supportive care?
Jason Hamed: We got to get corrective exercises into that person. So you’re talking about a bio hack is we have … and this was tough, because this isn’t a blanket one. This one, I can’t just say, hey just go do this one exercise because that’s not true, it’s not a one size fits all. I know where your weaknesses are and we work on those things and someone else may have different challenges. But, ultimately, once the alignment has reached its near optimal, once the disc has self-absorbed as best it possibly can, then what we have to do, we have to help that person create strength around the foundation and also take into account with their life stressors are and then build a protocol around that.
So I still advocate check-up adjustments moving forward to make sure that their alignment is holding. A periodic x-ray maybe once a year, so we can continue to monitor if they’re continuing to hold in alignment or did life go wonky on them and they went sideways again. But, in between those treatments, in between that checkup time, I want to empower that person with specific exercises that are fit for their life, their stressors, their demands, and where their weaknesses are.
Closing Thoughts: Take Care Of Your Back
Bryan Joseph: So let’s bring this full circle because the final phase in regards to what we’re talking about, there are exercises really to come back and protect the soft tissue, which is what we talked about earlier in this episode that was dealing with the micro trauma. So basically that scar tissue, that rigid tissue, the poor flexibility, the overstretched tissue, whatever it might be in terms of your muscles or your tendons, or your ligaments, that’s supporting the alignment, that is what needs to be rehabbed.
Very similar to when somebody gets their braces taken off of their teeth, that they basically put a retainer on. The closest thing to a retainer that your spinal structure has, is your core musculature and your soft tissue. So it’s very important to just not let that dissipate or weaken again, but to support it in between any one of your activities and keep it strong and healthy and vibrant and flexible.
Jason Hamed: Well said.
Bryan Joseph: So thank you for joining us again. If you liked this episode, clearly there’s a lot of people … It’s amazing the amount, the number of people that are experiencing back pain in today’s culture, and I know that lifestyle has a lot to do with that, but if you, yourself, or somebody else that you know is experiencing back issues, looking for help, it all starts with a conversation.
Check out our page for more of our podcasts.
